Tennis elbow
| Tennis elbow | |
|---|---|
| Other names | Lateral epicondylitis, lateral elbow tendinopathy[1], pickleball elbow[2], masturbator's elbow |
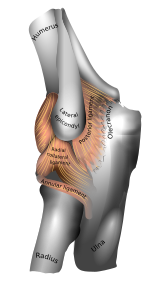 | |
| Left elbow-joint. (Lateral epicondyle visible at center.) | |
| Specialty | Orthopedics, sports medicine |
| Symptoms | Painful and tender outer part of the elbow[1] |
| Usual onset | Gradual[3] |
| Duration | Less than 1 to 2 years[4] |
| Causes | Middle age (ages 35-60). |
| Diagnostic method | Symptoms and physical examination |
| Differential diagnosis | Osteoarthritis |
| Treatment | Nothing is proved to alter the natural course of the disease. Exercises, braces, ice or heat, and medications may be palliative. |
Tennis elbow, also known as lateral epicondylitis is an enthesopathy (attachment point disease) of the origin of the extensor carpi radialis brevis on the lateral epicondyle.[1][5] It causes pain and tenderness over the bony part of the lateral epicondyle. Symptoms range from mild tenderness to severe, persistent pain.[1][6][7] The pain may also extend into the back of the forearm.[3] It usually has a gradual onset, but it can seem sudden and be misinterpreted as an injury.[8][3][9]
Tennis elbow is often idiopathic. Its cause and pathogenesis are unknown.[10] It likely involves tendinosis, a degeneration of the local tendon.[11][10]
It is thought this condition is caused by excessive use of the muscles of the back of the forearm, but this is not supported by evidence.[3][12] It may be associated with work or sports, classically racquet sports (including paddle sports), but most people with the condition are not exposed to these activities.[1][3][13] The diagnosis is based on the symptoms and examination. Medical imaging is not very useful.[3][10]
Untreated enthesopathy usually resolves in 1–2 years. Treating the symptoms and pain involves medications such as NSAIDS or acetaminophen, a wrist brace, or a strap over the upper forearm.[1][3] The role of corticosteroid injections as a form of treatment is still debated.[10] Recent studies suggests that corticosteroid injections may delay symptom resolution.[10]
Signs and symptoms
[edit]Patients typically feel pain or burning around the outer part of the elbow (lateral epicondyle of the humerus), which can move down the forearm and sometimes up to the upper arm.[10] The pain is worsened by activities that involve wrist extension, such as gripping objects.[14][15] Pain intensity varies from mild to severe and can be intermittent or constant, significantly impacting daily life. Patients also commonly report grip weakness and difficulty lifting.[16]
Terminology
[edit]The term "tennis elbow" is widely used (although informal), but the condition affects non-tennis players.[17][18] More recently, with the explosive growth of pickleball, the term "pickleball elbow" is frequently used.[2] Historically, the medical term "lateral epicondylitis" was most commonly used for the condition, but "itis" implies inflammation and the condition is not inflammatory.[7] It is also referred to as enthesopathy of the extensor carpi radialis origin.[5]
Since histological findings reveal noninflammatory tissue, the terms "lateral elbow tendinopathy" and "tendinosis" are suggested.[19][20] In 2019, a group of international experts suggested that "lateral elbow tendinopathy" was the most appropriate terminology.[21] But a disease of an attachment point (or enthesia) is most accurately referred to as an "enthesopathy."[22]
Causes
[edit]
The exact cause of lateral epicondylitis remains unclear. However, it is often linked to repetitive microtrauma resulting from excessive gripping, wrist extension, radial deviation, and/or forearm supination.[23][24]
Traditionally, people have speculated that tennis elbow is a type of repetitive strain injury resulting from tendon overuse and failed healing of the tendon, but there is no evidence of injury or repair, and misinterpretation of painful activities as a source of damage is common.[25]

Pathophysiology
[edit]The extensor carpi radialis brevis is the most commonly affected muscle in lateral epicondylitis (LE), along with other extensor carpal muscles.[15] Due to its unique origin, the ECRB tendon is prone to abrasion during elbow movements, leading to repetitive microtrauma.
Lateral epicondylitis was initially considered an inflammatory process, however there is no evidence of inflammation or repair.[26] Therefore, the disorder is more appropriately referred to as tendinosis or tendinopopathy.[19] Tendinosis, a degenerative condition with fibroblasts, abnormal collagen, and increased blood vessels. Repetitive stress causes microtears, scar tissue formation, and biomechanical changes, worsening symptoms over time.
Clinical evaluation
[edit]Physical examination
[edit]Diagnosis is based on symptoms and clinical signs that are discrete and characteristic. For example, the extension of the elbow and flexion of the wrist causes outer elbow pain. The physical examination usually reveals marked tenderness at the origin of the extensor carpi radialis brevis muscle from the lateral epicondyle (extensor carpi radialis brevis origin).[27] Pain may worsen with resisted wrist extension, middle finger extension, and forearm supination with an extended elbow, although normal elbow movement is often maintained, even in severe cases.[15]
Cozen's test
[edit]Cozen's test is a physical examination performed to evaluate for tennis elbow involving pain with resisted wrist extension.[28] The test is said to be positive if a resisted wrist extension triggers pain to the lateral aspect of the elbow owing to stress placed upon the tendon of the extensor carpi radialis brevis muscle.[29] The test is performed with extended elbow. NOTE: With elbow flexed the extensor carpi radialis longus is in a shortened position as its origin is the lateral supracondylar ridge of the humerus. To rule out the ECRB (extensor carpi radialis brevis), repeat the test with the elbow in full extension.
Medical imaging
[edit]Medical imaging is not necessary or helpful.[30]
Radiographs (X-rays) may demonstrate calcification where the extensor muscles attach to the lateral epicondyle.[27] Medical ultrasonography and magnetic resonance imaging (MRI) can demonstrate the pathology, but are not helpful for diagnosis and do not influence treatment.[31]
Longitudinal sonogram of the lateral elbow displays thickening and heterogeneity of the common extensor tendon that is consistent with tendinosis, as the ultrasound reveals calcifications, intrasubstance tears, and marked irregularity of the lateral epicondyle. Although the term “epicondylitis” is frequently used to describe this disorder, most histopathologic findings of studies have displayed no evidence of an acute, or a chronic inflammatory process. Histologic studies have demonstrated that this condition is the result of tendon degeneration, which replaces normal tissue with a disorganized arrangement of collagen. Colour Doppler ultrasound reveals structural tendon changes, with vascularity and hypo-echoic areas that correspond to the areas of pain in the extensor origin.[32]
Table of Clinical classification of lateral epicondylitis phases.[33]
| Phase | Description of pain changes at different phases |
|---|---|
| I | Mild pain after activity, usually recovers within 24 hours |
| II | Mild pain more than 48 hours after activity, no pain during activity, can be relieved with warm-up exercises, and recovers within 72 hours |
| III | Mild pain before and during activity, no significant negative impact on the activities, and can be partially relieved with warm-up exercises |
| IV | Mild pain accompanies the activities of daily living and has negative impact on the performance of activities |
| V | Harmful pain unrelated to activities, great negative impact on the performance of activities but does not prevent the activities of daily life. Need complete rest to control the pain |
| VI | Persistent pain despite complete rest and can prevent the activities of daily life |
| VII | Consistent pain at rest, aggravated after activities, and disturbed sleep |
Prevention
[edit]Activity modification is the best way to prevent the occurrence of lateral epicondylitis. Prevention can include avoiding extreme end range motions in extension and flexion, limit repetitive hand and wrist motions, and modification of heavy lifting with extended arms. Lifestyle factors such as smoking, alcohol drinking, and dietary habits are known to influence the prognosis of various medical conditions. Smokers showed a higher chance of developing lateral epicondylitis compared to non-smokers.[34][35] Current research indicates that alcohol intake is not significantly associated with lateral epicondylitis.[36]
Treatment
[edit]Non-Operative Treatment
[edit]Non operative treatment resolves 90% of symptomatic lateral epicondylitis.[37][38] Nonoperative care usually includes activity modification, physical therapy, non-steroidal anti-inflammatory medications, bracing, extracorporeal shock-wave therapy, and acupuncture. Modifying activity and avoiding overuse are key to treatment. Lifting with the palm up and avoiding palm-down movements can shift strain from the lateral to the medial epicondyle, easing pain.[37] Patients should also improve lifestyle habits and avoid triggering activities. Following the RICE method (rest, ice, compression, elevation) can help relieve pain initially.[38]
Exercises
[edit]Stretching and isometric strengthening are the most common recommended exercises.
The muscle is stretched with the elbow straight and the wrist passively flexed.
Isometric strengthening can be done by pushing the top of the hand up against the undersurface of a table and holding the wrist straight.[39]
Orthotic devices
[edit]

Orthosis is a device externally used on the limb to improve the function or reduce the pain. Orthotics may be useful in tennis elbow; however, long-term effects are unknown.[40] There are two main types of orthoses prescribed for this problem: counterforce elbow orthoses and wrist extension orthoses. Counterforce orthosis has a circumferential structure surrounding the arm. This orthosis usually has a strap which applies a binding force over the origin of the wrist extensors. The applied force by orthosis reduces the elongation within the musculotendinous fibers. Wrist extensor orthosis maintains the wrist in the slight extension.
Speculative treatments
[edit]Other approaches that are not experimentally tested include eccentric exercise using a rubber bar, joint manipulation directed at the elbow and wrist, spinal manipulation directed at the cervical and thoracic spinal regions, low level laser therapy, and extracorporeal shockwave therapy.[37][41][42][43][44]
Medication
[edit]Recent studies demonstrate that topical nonsteroidal anti-inflammatory medications are effective within four weeks for lateral epicondylitis.[45][46][10] Evidence for oral NSAIDs is mixed.[45] Research indicates that corticosteroid injections improved outcomes more effectively than NSAIDs within four weeks but offered no long-term benefits at 12 months.[38]
Other studies suggest that, while helpful for short-term pain relief, corticosteroid injections are less effective than watchful waiting or physical therapy after one year.[10] Repeated injections can also lead to tendon rupture and muscle atrophy. Thus, clinicians should be cautious with corticosteroid use for lateral epicondylitis due to limited long-term effectiveness and possible adverse effects.[47]
Alternative Treatments
[edit]While many alternative treatments, such as shockwave, laser, low-frequency electrical nerve stimulation, ultrasound, and pulsed magnetic wave therapies, have been used, none have been proven effective.[10][48][49] Current evidence is inconclusive on the effectiveness of acupuncture was effective for lateral epicondylitits.[50][51]
Platelet-Rich Plasma (PRP) Injections
[edit]Platelet-Rich Plasma (PRP) has emerged as a potential treatment for lateral epicondylitis. PRP is derived from the patient's own blood and contains concentrated platelets, which are rich in growth factors.[52] These growth factors are believed to initiate and accelerate tissue repair and regeneration support healing of the tendons and connective tissue and promote the growth of new blood vessels, aiding the recovery process.[52]
The PRP procedure for lateral epicondylitis involves extracting a small amount of the patient's blood, separating the plasma through centrifugation, and re-injecting it directly into the lateral epicondyle.[53] While good outcomes have been reported with PRP for lateral epicondylitis,[53] the overall literature is still unclear on its effectiveness.[54] Additionally, variations in PRP preparation methods and injection techniques across different commercial systems add further complexity to assessing its effectiveness.
Overall, current research on PRP as a treatment for lateral epicondylitis is promising. However, more studies are needed to provide clear evidence of its effectiveness.[7]
Surgery
[edit]Most patients with lateral epicondylitis (tennis elbow) improve with conservative treatments and do not need surgery. However, if symptoms persist despite prolonged conservative therapy, surgical options should be reconsidered.[55] Several surgical procedures are available for lateral epicondylitis, most involving the removal of damaged tissue from the ECRB and scraping of the lateral epicondyle. This procedure can be done through open, percutaneous, or arthroscopic methods.[56][55][57]
Percutaneous Surgery
[edit]Percutaneous surgical approach is mainly used for releasing the common extensor tendon origin at the lateral epicondyle. This technique has been demonstrated to be safe, reliable, and cost-effective[10][58] Good midterm outcomes in pain relief have been widely reported with a percutaneous surgical approach.[10] However there is some limited evidence reported that arthroscopic and open techniques achieved a better prognosis than the percutaneous surgical approach for the treatment of lateral epicondylitis.[59] In recent years, a new technique termed as ultrasound-guided percutaneous tenotomy has been reported as a safe and effective for the treatment of lateral epicondylitis, with improvements in symptoms, function, and ultrasound imaging at 1-year follow-up.[60]
Arthroscopic Surgery
[edit]Arthroscopic surgery is a minimally invasive option for treating lateral epicondylitis. This technique fully visualizes the elbow joint, and leads to a quicker return to work.[59] In the past, studies have shown good long term effects and fewer complications with arthroscopic surgery compared to open or percutaneous approaches.[59] However, the literature is currently mixed with some recent reviews suggest no significant differences among open, arthroscopic, and percutaneous methods regarding recovery time, complication rates, or patient satisfaction.[61][59] While others state that arthroscopic surgery may allow for a quicker return to work, suggesting a potential advantage in the early postoperative period.[62] While results are generally positive, arthroscopic surgery carries risks of injury to the radial nerve and lateral ulnar collateral ligament.
Epidemiology
[edit]Tennis Elbow is a commonly seen condition and has been reported to affect 1% to 3% of adults each year.[63][64] The incidence of lateral elbow tendinosis has declined, which could be due to shifts in diagnostic practices or an actual drop in cases.[65] Understanding the typical disease progression can help patients and providers choose the best treatment approach.
Symptoms of lateral epicondylitis
[edit]Symptoms suggestive of lateral epicondylitis are present in about 1% of the adult population and are most common between ages 40 and 60.[66] The prevalence varies somewhat between studies, likely as a result of varied diagnostic criteria and limited reliability between different observers.[66] The data regarding symptoms of lateral epicondylitis in relation to occupations and sports are inconsistent and inconclusive.[66] The shortcomings of the evidence that addresses the relationship between symptoms and occupation/sport include: variation in diagnostic criteria, limited reliability of diagnosis, confounding association of psychosocial factors, selection bias due to a high non-response rate, and the fact that exposures are usually by subjective patient reports and symptomatic patients might receive greater exposure.[66]
History
[edit]German physician F. Runge[67] is usually credited for the first description of the condition, calling it "writer's cramp" (Schreibekrampf) in 1873.[68] Later, it was called as "washer women's elbow".[69] British surgeon Henry Morris published an article in The Lancet describing "lawn tennis arm" in 1883.[70][67] The popular term "tennis elbow" first appeared the same year in a paper by H. P. Major, described as "lawn-tennis elbow".[71][72]
See also
[edit]References
[edit]- ^ a b c d e f Hubbard MJ, Hildebrand BA, Battafarano MM, Battafarano DF (June 2018). "Common Soft Tissue Musculoskeletal Pain Disorders". Primary Care. 45 (2): 289–303. doi:10.1016/j.pop.2018.02.006. PMID 29759125. S2CID 46886582.
- ^ a b Godman, Heidi (September 1, 2023). "How to avoid this common pickleball injury". health.harvard.edu. Harvard Health Publishing. Archived from the original on June 19, 2024. Retrieved 28 November 2024.
- ^ a b c d e f g "Tennis Elbow (Lateral Epicondylitis)". OrthoInfo. July 2015. Retrieved 21 June 2018.
- ^ Vaquero-Picado A, Barco R, Antuña SA (November 2016). "Lateral epicondylitis of the elbow". EFORT Open Reviews. 1 (11): 391–397. doi:10.1302/2058-5241.1.000049. PMC 5367546. PMID 28461918.
- ^ a b Faro, Frances; Wolf, Jennifer Moriatis (October 2007). "Lateral Epicondylitis: Review and Current Concepts". The Journal of Hand Surgery. 32 (8): 1271–1279. doi:10.1016/j.jhsa.2007.07.019. ISSN 0363-5023. PMID 17923315.
- ^ Behazin M, Kachooei AR (March 2021). "Arthroscopic Recession Technique in the Surgery of Tennis Elbow by Sharp Cutting the Extensor Carpi Radialis Brevis (ECRB) Tendon Origin". The Archives of Bone and Joint Surgery. 9 (2): 174–179. doi:10.22038/abjs.2020.48173.2383. PMC 8121031. PMID 34026934.
- ^ a b c Cutts, S.; Gangoo, Shafat; Modi, Nitin; Pasapula, Chandra (2020). "Tennis elbow: A clinical review article". Journal of Orthopaedics. 17: 203–207. doi:10.1016/j.jor.2019.08.005. ISSN 0972-978X. PMC 6926298. PMID 31889742.
- ^ Lemmers, M.; Versluijs, Y.; Kortlever, J.; Gonzalez, A.; Ring, D. (2020). "Misperception of Disease Onset in People with Gradual-Onset Disease of the Upper Extremity". The Journal of Bone and Joint Surgery. 102 (24): 2174–2180. doi:10.2106/JBJS.20.00420. hdl:1887/3638637. PMID 33027085. S2CID 222211926.
- ^ Solheim E, Hegna J, Øyen J (June 2011). "Extensor tendon release in tennis elbow: results and prognostic factors in 80 elbows". Knee Surgery, Sports Traumatology, Arthroscopy. 19 (6): 1023–1027. doi:10.1007/s00167-011-1477-1. PMC 3096769. PMID 21409461.
- ^ a b c d e f g h i j k Ma, Kun-Long; Wang, Hai-Qiang (2020). "Management of Lateral Epicondylitis: A Narrative Literature Review". Pain Research & Management. 2020: 6965381. doi:10.1155/2020/6965381. PMC 7222600. PMID 32454922.
- ^ Gorski JM (August 2019). "Evaluation of Sleep Position for Possible Nightly Aggravation and Delay of Healing in Tennis Elbow". Journal of the American Academy of Orthopaedic Surgeons. Global Research & Reviews. 3 (8): e082. doi:10.5435/JAAOSGlobal-D-19-00082. PMC 6754212. PMID 31592507.
- ^ Bunata RE, Brown DS, Capelo R (September 2007). "Anatomic factors related to the cause of tennis elbow". The Journal of Bone and Joint Surgery. American Volume. 89 (9): 1955–1963. doi:10.2106/JBJS.F.00727. PMID 17768192.
- ^ "Mouse Elbow - Injury Overview". 17 May 2017.
- ^ Hsu, Stephanie H.; Moen, Todd C.; Levine, William N.; Ahmad, Christopher S. (March 2012). "Physical examination of the athlete's elbow". The American Journal of Sports Medicine. 40 (3): 699–708. doi:10.1177/0363546511428869. ISSN 1552-3365. PMID 22156170.
- ^ a b c Ahmad, Z.; Siddiqui, N.; Malik, S. S.; Abdus-Samee, M.; Tytherleigh-Strong, G.; Rushton, N. (March 2013). "Lateral epicondylitis: a review of pathology and management". The Bone & Joint Journal. 95-B (9): 1158–1164. doi:10.1302/0301-620X.95B9.29285. ISSN 2049-4408. PMID 23997125.
- ^ Dorf, Erik R.; Chhabra, A. Bobby; Golish, S. Raymond; McGinty, Jasmin L.; Pannunzio, Michael E. (2007). "Effect of elbow position on grip strength in the evaluation of lateral epicondylitis". The Journal of Hand Surgery. 32 (6): 882–886. doi:10.1016/j.jhsa.2007.04.010. ISSN 0363-5023. PMID 17606071.
- ^ "Tennis elbow (lateral epicondylitis) Elbow Pain". Cleveland Clinic. 2018. Retrieved 23 January 2018.
- ^ "Tennis elbow". Mayo Clinic. 2 August 2017. Retrieved 23 January 2018.
- ^ a b McShane JM, Nazarian LN, Harwood MI (October 2006). "Sonographically guided percutaneous needle tenotomy for treatment of common extensor tendinosis in the elbow". Journal of Ultrasound in Medicine. 25 (10): 1281–1289. doi:10.7863/jum.2006.25.10.1281. PMID 16998100. S2CID 22963436.
- ^ du Toit C, Stieler M, Saunders R, Bisset L, Vicenzino B (November 2008). "Diagnostic accuracy of power Doppler ultrasound in patients with chronic tennis elbow". British Journal of Sports Medicine. 42 (11): 872–876. doi:10.1136/bjsm.2007.043901. hdl:10072/22142. PMID 18308874. S2CID 3274396.
- ^ Scott A, Squier K, Alfredson H, Bahr R, Cook JL, Coombes B, et al. (March 2020). "ICON 2019: International Scientific Tendinopathy Symposium Consensus: Clinical Terminology". British Journal of Sports Medicine. 54 (5): 260–262. doi:10.1136/bjsports-2019-100885. hdl:10397/97289. PMID 31399426. S2CID 199517946.
- ^ Ikonen J, Lähdeoja T, Ardern CL, Buchbinder R, Reito A, Karjalainen T (April 2022). "Persistent Tennis Elbow Symptoms Have Little Prognostic Value: A Systematic Review and Meta-analysis". Clinical Orthopaedics and Related Research. 480 (4): 647–660. doi:10.1097/CORR.0000000000002058. PMC 8923574. PMID 34874323.
- ^ Eygendaal, Denise; Rahussen, F. Th G.; Diercks, R. L. (November 2007). "Biomechanics of the elbow joint in tennis players and relation to pathology". British Journal of Sports Medicine. 41 (11): 820–823. doi:10.1136/bjsm.2007.038307. ISSN 1473-0480. PMC 2465285. PMID 17638843.
- ^ Lee, Han-Sung; Park, Ho Youn; Yoon, Jun O.; Kim, Jin Sam; Chun, Jae Myeung; Aminata, Iman W.; Cho, Won-Joon; Jeon, In-Ho (September 2013). "Musicians' medicine: musculoskeletal problems in string players". Clinics in Orthopedic Surgery. 5 (3): 155–160. doi:10.4055/cios.2013.5.3.155. ISSN 2005-4408. PMC 3758983. PMID 24009899.
- ^ Gunn CC, Milbrandt WE (May 1976). "Tennis elbow and the cervical spine". Canadian Medical Association Journal. 114 (9): 803–809. PMC 1957126. PMID 1268791.
- ^ Nirschl RP, Ashman ES (2004-01-01). "Tennis elbow tendinosis (epicondylitis)". Instructional Course Lectures. 53: 587–598. PMID 15116648.
- ^ a b Sarwark JF (2010). Essentials of musculoskeletal care. Rosemont, Ill.: American Academy of Orthopaedic Surgeons. ISBN 978-0892035793. OCLC 706805938.
- ^ Uttamchandani, Shivani R.; Phansopkar, Pratik (2024). "Conservative Management of Lateral Epicondylalgia: A Review". Cureus. 16 (5): e59875. doi:10.7759/cureus.59875. ISSN 2168-8184. PMC 11157989. PMID 38854316.
- ^ Cooper G (2007-10-28). Pocket Guide to Musculoskeletal Diagnosis. Springer Science & Business Media. pp. 44–. ISBN 978-1-59745-009-6.
- ^ Orchard J, Kountouris A (May 2011). "The management of tennis elbow". BMJ. 342: d2687. doi:10.1136/bmj.d2687. PMID 21558359. S2CID 8358075.
- ^ Keijsers R, de Vos RJ, Kuijer PP, van den Bekerom MP, van der Woude HJ, Eygendaal D (October 2019). "Tennis elbow". Shoulder & Elbow. 11 (5): 384–392. doi:10.1177/1758573218797973. PMC 6739751. PMID 31534489.
- ^ du Toit C, Stieler M, Saunders R, Bisset L, Vicenzino B (November 2008). "Diagnostic accuracy of power Doppler ultrasound in patients with chronic tennis elbow". British Journal of Sports Medicine. 42 (11): 872–876. doi:10.1136/bjsm.2007.043901. hdl:10072/22142. PMID 18308874. S2CID 3274396.
- ^ Nirschl, Robert P.; Ashman, Edward S. (October 2003). "Elbow tendinopathy: tennis elbow". Clinics in Sports Medicine. 22 (4): 813–836. doi:10.1016/s0278-5919(03)00051-6. ISSN 0278-5919. PMID 14560549.
- ^ Marigi, Erick M.; Dancy, Malik; Alexander, Andrew; Marigi, Ian M.; Clark, Julian; Krych, Aaron J.; Camp, Christopher L.; Okoroha, Kelechi R. (2023-02-01). "Lateral Epicondylitis: Critical Analysis Review of Current Nonoperative Treatments". JBJS Reviews. 11 (2). doi:10.2106/JBJS.RVW.22.00170. ISSN 2329-9185. PMID 36800442.
- ^ Park, Hyung Bin; Gwark, Ji-Yong; Im, Jin-Hyung; Na, Jae-Boem (May 2021). "Factors Associated With Lateral Epicondylitis of the Elbow". Orthopaedic Journal of Sports Medicine. 9 (5): 23259671211007734. doi:10.1177/23259671211007734. ISSN 2325-9671. PMC 8127791. PMID 34036114.
- ^ Otoshi, Kenichi; Takegami, Misa; Sekiguchi, Miho; Onishi, Yoshihiro; Yamazaki, Shin; Otani, Koji; Shishido, Hiroaki; Fukuhara, Shunichi; Kikuchi, Shinichi; Konno, Shinichi (2015). "Chronic hyperglycemia increases the risk of lateral epicondylitis: the Locomotive Syndrome and Health Outcome in Aizu Cohort Study (LOHAS)". SpringerPlus. 4: 407. doi:10.1186/s40064-015-1204-3. ISSN 2193-1801. PMC 4530269. PMID 26266078.
- ^ a b c Hoogvliet, Peter; Randsdorp, Manon S.; Dingemanse, Rudi; Koes, Bart W.; Huisstede, Bionka M. A. (November 2013). "Does effectiveness of exercise therapy and mobilisation techniques offer guidance for the treatment of lateral and medial epicondylitis? A systematic review". British Journal of Sports Medicine. 47 (17): 1112–1119. doi:10.1136/bjsports-2012-091990. ISSN 1473-0480. PMID 23709519.
- ^ a b c Hay, E. M.; Paterson, S. M.; Lewis, M.; Hosie, G.; Croft, P. (1999-10-09). "Pragmatic randomised controlled trial of local corticosteroid injection and naproxen for treatment of lateral epicondylitis of elbow in primary care". BMJ (Clinical Research Ed.). 319 (7215): 964–968. doi:10.1136/bmj.319.7215.964. ISSN 0959-8138. PMC 28251. PMID 10514160.
- ^ Santiago AO, Rios-Russo JL, Baerga L, Micheo W (2021-12-01). "Evidenced-Based Management of Tennis Elbow". Current Physical Medicine and Rehabilitation Reports. 9 (4): 186–194. doi:10.1007/s40141-021-00322-7. ISSN 2167-4833. S2CID 239460609.
- ^ Struijs PA, Smidt N, Arola H, Dijk C, Buchbinder R, Assendelft WJ (2002-01-21). "Orthotic devices for the treatment of tennis elbow". The Cochrane Database of Systematic Reviews. 2010 (1): CD001821. doi:10.1002/14651858.cd001821. PMC 8407516. PMID 11869609.
- ^ Tyler TF, Thomas GC, Nicholas SJ, McHugh MP (September 2010). "Addition of isolated wrist extensor eccentric exercise to standard treatment for chronic lateral epicondylosis: a prospective randomized trial". Journal of Shoulder and Elbow Surgery. 19 (6): 917–922. doi:10.1016/j.jse.2010.04.041. PMID 20579907.
- ^ Vicenzino B, Cleland JA, Bisset L (2007-01-01). "Joint manipulation in the management of lateral epicondylalgia: a clinical commentary". The Journal of Manual & Manipulative Therapy. 15 (1): 50–56. doi:10.1179/106698107791090132. PMC 2565595. PMID 19066643.
- ^ Herd CR, Meserve BB (2008-10-01). "A systematic review of the effectiveness of manipulative therapy in treating lateral epicondylalgia". The Journal of Manual & Manipulative Therapy. 16 (4): 225–237. doi:10.1179/106698108790818288. PMC 2716156. PMID 19771195.
- ^ Bjordal JM, Lopes-Martins RA, Joensen J, Couppe C, Ljunggren AE, Stergioulas A, Johnson MI (May 2008). "A systematic review with procedural assessments and meta-analysis of low level laser therapy in lateral elbow tendinopathy (tennis elbow)". BMC Musculoskeletal Disorders. 9 (1): 75. doi:10.1186/1471-2474-9-75. PMC 2442599. PMID 18510742.
- ^ a b Burnham, R.; Gregg, R.; Healy, P.; Steadward, R. (April 1998). "The effectiveness of topical diclofenac for lateral epicondylitis". Clinical Journal of Sport Medicine: Official Journal of the Canadian Academy of Sport Medicine. 8 (2): 78–81. doi:10.1097/00042752-199804000-00002. ISSN 1050-642X. PMID 9641433.
- ^ Spacca, G.; Cacchio, A.; Forgács, A.; Monteforte, P.; Rovetta, G. (2005). "Analgesic efficacy of a lecithin-vehiculated diclofenac epolamine gel in shoulder periarthritis and lateral epicondylitis: a placebo-controlled, multicenter, randomized, double-blind clinical trial". Drugs Under Experimental and Clinical Research. 31 (4): 147–154. ISSN 0378-6501. PMID 16223204.
- ^ Coombes, Brooke K.; Bisset, Leanne; Brooks, Peter; Khan, Asad; Vicenzino, Bill (2013-02-06). "Effect of corticosteroid injection, physiotherapy, or both on clinical outcomes in patients with unilateral lateral epicondylalgia: a randomized controlled trial". JAMA. 309 (5): 461–469. doi:10.1001/jama.2013.129. hdl:10072/55521. ISSN 1538-3598. PMID 23385272.
- ^ Weber, Christoph; Thai, Veronika; Neuheuser, Katrin; Groover, Katharina; Christ, Oliver (2015-08-25). "Efficacy of physical therapy for the treatment of lateral epicondylitis: a meta-analysis". BMC Musculoskeletal Disorders. 16: 223. doi:10.1186/s12891-015-0665-4. ISSN 1471-2474. PMC 4549077. PMID 26303397.
- ^ D'Angelo, Kevin; Sutton, Deborah; Côté, Pierre; Dion, Sarah; Wong, Jessica J.; Yu, Hainan; Randhawa, Kristi; Southerst, Danielle; Varatharajan, Sharanya; Cox Dresser, Jocelyn; Brown, Courtney; Menta, Roger; Nordin, Margareta; Shearer, Heather M.; Ameis, Arthur (September 2015). "The effectiveness of passive physical modalities for the management of soft tissue injuries and neuropathies of the wrist and hand: a systematic review by the Ontario Protocol for Traffic Injury Management (OPTIMa) collaboration". Journal of Manipulative and Physiological Therapeutics. 38 (7): 493–506. doi:10.1016/j.jmpt.2015.06.006. ISSN 1532-6586. PMID 26303967.
- ^ Tang, Hongzhi; Fan, Huaying; Chen, Jiao; Yang, Mingxiao; Yi, Xuebing; Dai, Guogang; Chen, Junrong; Tang, Liugang; Rong, Haibo; Wu, Junhua; Liang, Fanrong (2015). "Acupuncture for Lateral Epicondylitis: A Systematic Review". Evidence-Based Complementary and Alternative Medicine: ECAM. 2015: 861849. doi:10.1155/2015/861849. ISSN 1741-427X. PMC 4710923. PMID 26843886.
- ^ Buchbinder, Rachelle; Green, Sally Elizabeth; Struijs, Peter (2008-05-28). "Tennis elbow". BMJ Clinical Evidence. 2008: 1117. ISSN 1752-8526. PMC 2907994. PMID 19450309.
- ^ a b Everts, Peter; Onishi, Kentaro; Jayaram, Prathap; Lana, José Fábio; Mautner, Kenneth (2020-10-21). "Platelet-Rich Plasma: New Performance Understandings and Therapeutic Considerations in 2020". International Journal of Molecular Sciences. 21 (20): 7794. doi:10.3390/ijms21207794. ISSN 1422-0067. PMC 7589810. PMID 33096812.
- ^ a b Mishra, Allan; Pavelko, Terri (November 2006). "Treatment of chronic elbow tendinosis with buffered platelet-rich plasma". The American Journal of Sports Medicine. 34 (11): 1774–1778. doi:10.1177/0363546506288850. ISSN 0363-5465. PMID 16735582.
- ^ Thanasas, Christos; Papadimitriou, George; Charalambidis, Charalambos; Paraskevopoulos, Ilias; Papanikolaou, Athanasios (October 2011). "Platelet-rich plasma versus autologous whole blood for the treatment of chronic lateral elbow epicondylitis: a randomized controlled clinical trial". The American Journal of Sports Medicine. 39 (10): 2130–2134. doi:10.1177/0363546511417113. ISSN 1552-3365. PMID 21813443.
- ^ a b Lo MY, Safran MR (October 2007). "Surgical treatment of lateral epicondylitis: a systematic review". Clinical Orthopaedics and Related Research. 463: 98–106. doi:10.1097/BLO.0b013e3181483dc4. PMID 17632419. S2CID 6954029.
- ^ Monto R (September 2014). "Tennis elbow repair with or without suture anchors: a randomized clinical trial". Techniques in Shoulder and Elbow Surgery. 15 (3): 92–97. doi:10.1097/BTE.0000000000000027. S2CID 58020081.
- ^ Solheim E, Hegna J, Øyen J (May 2013). "Arthroscopic versus open tennis elbow release: 3- to 6-year results of a case-control series of 305 elbows". Arthroscopy. 29 (5): 854–859. doi:10.1016/j.arthro.2012.12.012. PMID 23388420.
- ^ Kaleli, Tufan; Ozturk, Cagatay; Temiz, Aytun; Tirelioglu, Onur (April 2004). "Surgical treatment of tennis elbow: percutaneous release of the common extensor origin". Acta Orthopaedica Belgica. 70 (2): 131–133. ISSN 0001-6462. PMID 15165014.
- ^ a b c d Pierce, Todd P.; Issa, Kimona; Gilbert, Benjamin T.; Hanly, Brian; Festa, Anthony; McInerney, Vincent K.; Scillia, Anthony J. (June 2017). "A Systematic Review of Tennis Elbow Surgery: Open Versus Arthroscopic Versus Percutaneous Release of the Common Extensor Origin". Arthroscopy: The Journal of Arthroscopic & Related Surgery: Official Publication of the Arthroscopy Association of North America and the International Arthroscopy Association. 33 (6): 1260–1268.e2. doi:10.1016/j.arthro.2017.01.042. ISSN 1526-3231. PMID 28412059.
- ^ Koh, Joyce S. B.; Mohan, P. C.; Howe, T. S.; Lee, Brian P.; Chia, S. L.; Yang, Zixian; Morrey, Bernard F. (March 2013). "Fasciotomy and surgical tenotomy for recalcitrant lateral elbow tendinopathy: early clinical experience with a novel device for minimally invasive percutaneous microresection". The American Journal of Sports Medicine. 41 (3): 636–644. doi:10.1177/0363546512470625. ISSN 1552-3365. PMID 23302261.
- ^ Burn, Matthew B.; Mitchell, Ronald J.; Liberman, Shari R.; Lintner, David M.; Harris, Joshua D.; McCulloch, Patrick C. (May 2018). "Open, Arthroscopic, and Percutaneous Surgical Treatment of Lateral Epicondylitis: A Systematic Review". Hand (New York, N.Y.). 13 (3): 264–274. doi:10.1177/1558944717701244. ISSN 1558-9455. PMC 5987981. PMID 28720043.
- ^ Ghandour, Maher; Al Salloum, Diaa; Jaber, Mohamad Houssein; Abou Orm, Ghadi; Ghosn, Ali; Jaber, Sadek; Abd El Nour, Hicham; Chalfoun, Anthony; Dagher, Tanios; Hanna, Bashour (January 2025). "A comparative meta-analysis of the efficacy and safety of arthroscopic versus open surgery in patients with lateral epicondylitis". Journal of Orthopaedics. 59: 41–50. doi:10.1016/j.jor.2024.07.018. ISSN 0972-978X. PMC 11439539. PMID 39351266.
- ^ Calfee, Ryan P.; Patel, Amar; DaSilva, Manuel F.; Akelman, Edward (January 2008). "Management of lateral epicondylitis: current concepts". The Journal of the American Academy of Orthopaedic Surgeons. 16 (1): 19–29. doi:10.5435/00124635-200801000-00004. ISSN 1067-151X. PMID 18180389.
- ^ Verhaar, J. A. (October 1994). "Tennis elbow. Anatomical, epidemiological and therapeutic aspects". International Orthopaedics. 18 (5): 263–267. doi:10.1007/BF00180221. ISSN 0341-2695. PMID 7852001.
- ^ Sanders, Thomas L.; Maradit Kremers, Hilal; Bryan, Andrew J.; Ransom, Jeanine E.; Smith, Jay; Morrey, Bernard F. (May 2015). "The epidemiology and health care burden of tennis elbow: a population-based study". The American Journal of Sports Medicine. 43 (5): 1066–1071. doi:10.1177/0363546514568087. ISSN 1552-3365. PMC 4517446. PMID 25656546.
- ^ a b c d Shiri R, Viikari-Juntura E (February 2011). "Lateral and medial epicondylitis: role of occupational factors". Best Practice & Research. Clinical Rheumatology. 25 (1): 43–57. doi:10.1016/j.berh.2011.01.013. PMID 21663849.
- ^ a b "Tennis Elbow-Cap". The Lancet. 128 (3301): 1083. 1886. doi:10.1016/s0140-6736(00)49587-5.
- ^ Runge F (1873). "Zur Genese und Behandlung des Schreibekrampfes". Berliner Klin Wochenschr. 10: 245–248.
- ^ Renstrom PA (5 November 2013). "Elbow Injuries in Tennis". In Reilly T, Hughes M, Lees A (eds.). Science and Racket Sports. E & FN Spon. ISBN 978-0-419-18500-0.
- ^ Flatt AE (October 2008). "Tennis elbow". Proceedings. 21 (4): 400–402. doi:10.1080/08998280.2008.11928437. PMC 2566914. PMID 18982084.
- ^ Major HP (1883). "Lawn-tennis elbow". BMJ. 2 (1185): 556–558. doi:10.1136/bmj.2.1185.556. PMC 2372911.
- ^ Kaminsky SB, Baker CL (December 2003). "Lateral epicondylitis of the elbow". Techniques in Hand & Upper Extremity Surgery. 7 (4): 179–189. doi:10.1097/00130911-200312000-00009. PMID 16518219. S2CID 128648.
External links
[edit]- Wilson JJ, Best TM (September 2005). "Common overuse tendon problems: A review and recommendations for treatment". American Family Physician. 72 (5): 811–818. PMID 16156339. Archived from the original on 2007-09-29. Retrieved 2006-03-11.
